LOS ANGELES – mPulse Mobile, a leader in conversational AI and digital engagement solutions, announces collaborations with over 30 managed healthcare organization customers to leverage digital engagement strategies to support the redetermination of Medicaid and CHIP enrollees following the end of the continuous enrollment period that was part of the Covid-19 public health emergency (PHE). These collaborations will ensure millions of low-income Americans retain the health coverage they need, and will provide digital resources to help individuals who no longer qualify for Medicaid transition to public exchange plans.
On December 29, 2022, President Biden signed a federal spending bill containing legislation decoupling continuous enrollment from the PHE effective April 1, 2023. Medicaid and CHIP enrollees will have to go through the recertification process to retain coverage. Medicaid Managed Care organizations (MCOs) have a 12-month timeframe to initiate and two additional months to complete renewals for their members in collaboration with local and state agencies. On January 23, 2023, the FCC issued a declaratory ruling reaffirming that the provision of a mobile phone number by a member to their state agency during the enrollment process constitutes prior express consent. Therefore, text outreach is an effective tool to drive the recertification process.
“Medicaid plans face a large administrative challenge to ensure their enrollees have continuous access to care,” said Bob Farrell, CEO of mPulse Mobile. “Many Medicaid beneficiaries tend to change addresses frequently, so traditional mailed recertification communications are less effective, whereas mobile phone ownership is well above 90% and text is utilized across populations. mPulse has pioneered the use of text outreach across lower income populations and individuals who face SDoH impacts, and we’ve consistently demonstrated our ability to engage and activate these hard-to-reach populations to take positive action for their own health.”
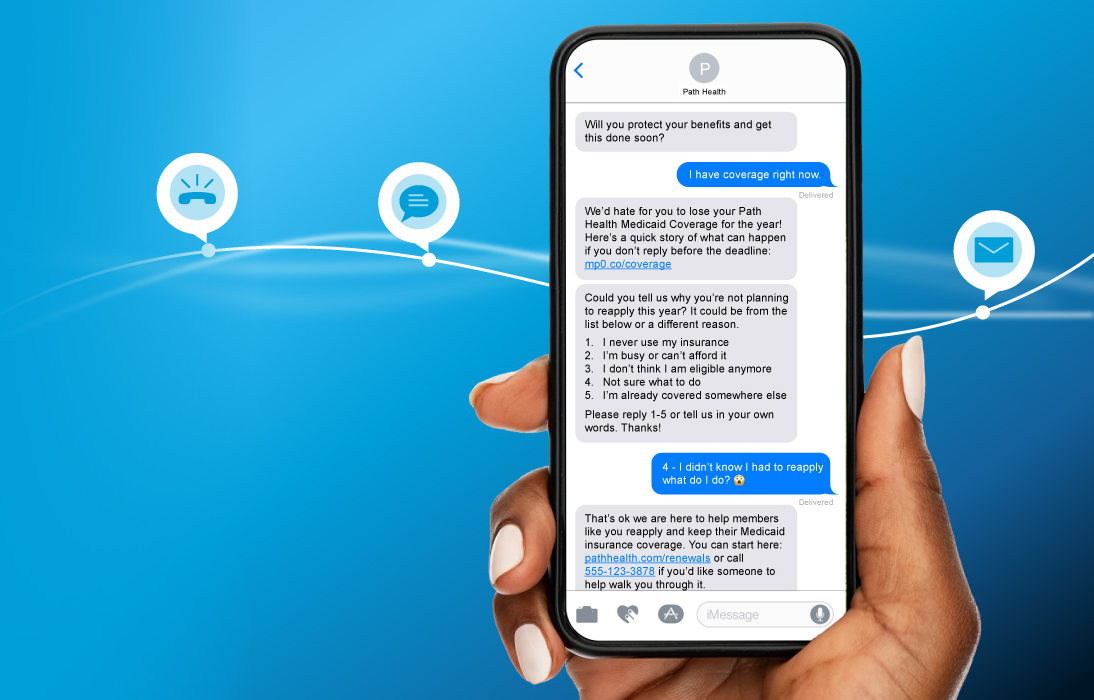
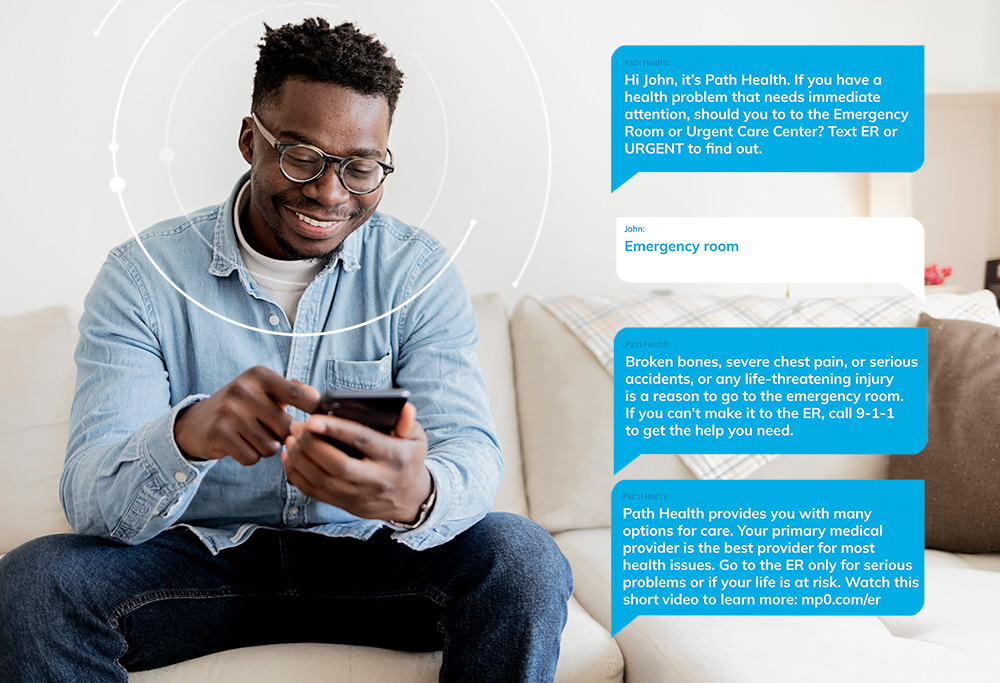
mPulse is working with a broad set of national and regional MCOs to deploy digital outreach programs to support members through the recertification process. mPulse’s conversational AI capabilities allow health plans to send out reminders with embedded links to online sites for recertification and ask questions about barriers that may be preventing members from re-enrolling. As members respond via text, the automated program addresses the issues they identify, which provides a robust consumer experience and improves program outcomes. mPulse has deployed automated conversational programs to Medicaid populations across seven languages. Prior to the Covid-19 pandemic, mPulse’s digital outreach redetermination programs consistently delivered over 20 percentage point improvements in redetermination rates compared to traditional communication channels.
“With much of the last year spent in a holding pattern with each 90-day PHE renewal, we finally have a clear path through the end of the unwinding phase,” said Reva Sheehan, Senior Director of Customer Insights at mPulse Mobile. “However, that doesn’t mean it will be easy. This is an all-hands-on-deck moment for Medicaid MCOs. We encourage all impacted health plans to take advantage of CMS’ call for states and MCOs to work together, and the FCC’s clarification of prior express consent to text and call individuals to provide assistance through the entire recertification process. In addition to known challenges and barriers, many of these individuals have never been through a recertification process. The robust multi-channel communication approach that mPulse Mobile provides is the best way to keep at-risk members from slipping through the cracks.”