mPulse Mobile recently wrapped up its fifth annual Activate conference with the Activate Awards, which provided yet another celebration of healthcare leadership, innovative program design, and improved health outcomes amidst various health engagement challenges.

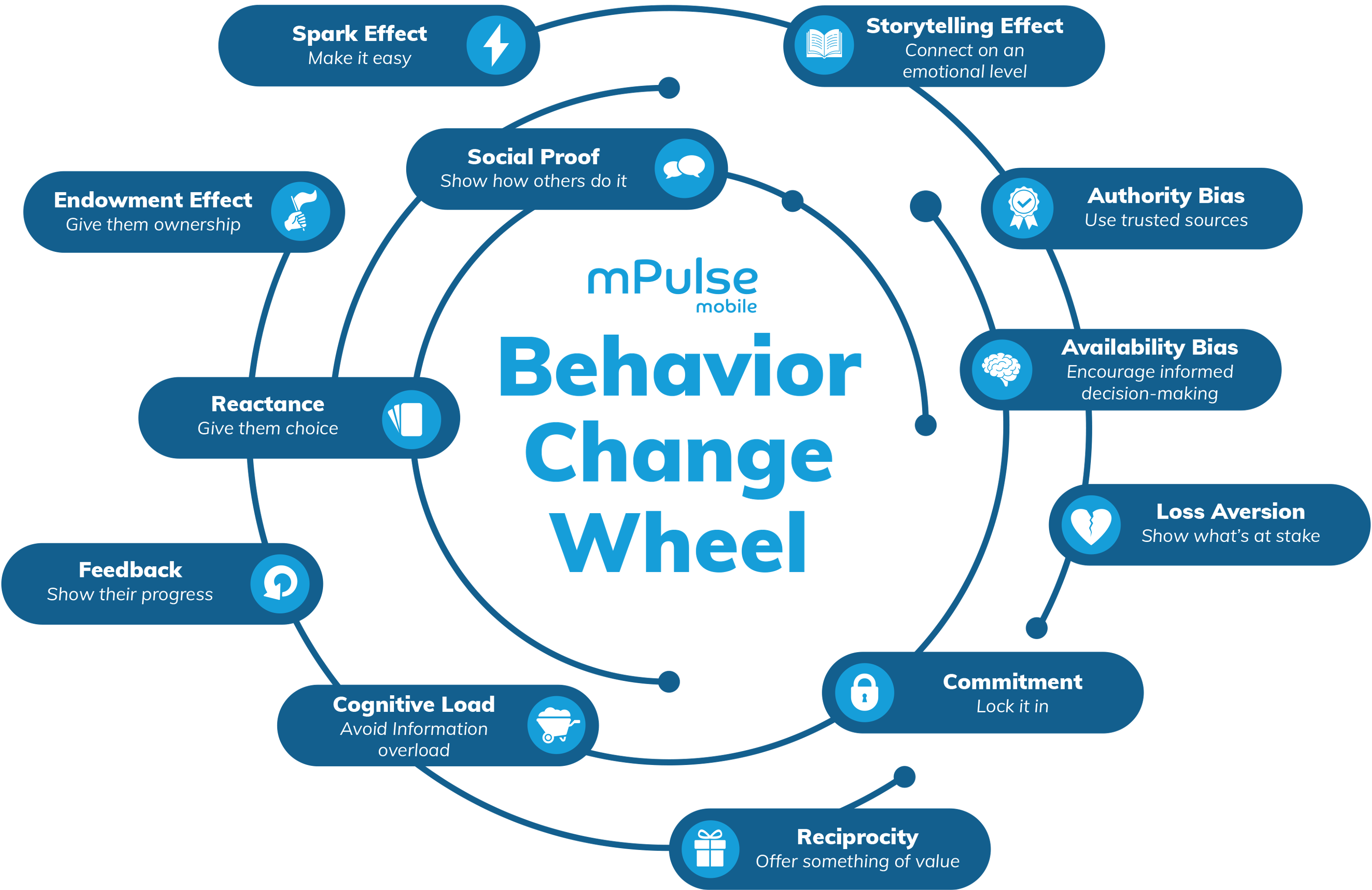
The theme of Activate2022, The Power of Behavioral Science to Drive Health Action, was reflected throughout the conference with captivating speaker sessions and expert panel discussions. Networking inspired exciting conversation around innovative technology, behavior change design, and consumer experience, and the Activate Awards surely brought those conversations full circle.
The awards help illuminate health plans, health systems, health service providers, PBMs and other types of healthcare organizations that utilized new strategies or unique tools to activate their consumer populations. The companies highlighted each year typically face barriers with engaging a certain population or driving specific health actions, so they search for innovative solutions to tackle those challenges.
For example, in 2019, CountyCare saw drastic rates of members losing Medicaid coverage, so the managed care organization (MCO) implemented automated text dialogues and saw their Redetermination rates improve by 3.3 percentage points in just one month, subsequently running away with the Most Improved Consumer Experience award. Last year, CareSource incorporated secure surveys, SMS, and streaming video to significantly impact their hard-to-reach members – they won 2021’s Best Use of Conversational A.I.
The same story is true for this year’s winners.
The remaining 3 award categories are Achieving Health Equity, Most Innovative Solution and Most Significant Outcome. Like the teamwork and critical thinking generated from breakout workshops and Q&A during the conference, the awards are a celebration of two companies that partnered together to overcome consumer barriers or gaps in care by building uniquely tailored engagement programs.
Here are the winners of the 2022 Activate Awards:
Achieving Health Equity
Program Goal
Increase Colorectal Cancer Screenings
AltaMed Health Services is one of the largest Federally Qualified Health Centers (FQHC) in the United States and provides a range of health services to Latino, multi-ethnic and underserved communities in Southern California. After seeing a steep drop in colorectal cancer screenings during the COVID-19 pandemic, the health center sought a solution that could help patients overcome barriers like language and lack of awareness of services.

AltaMed partnered with mPulse to deliver multi-lingual, educational health content to patients using mobile fotonovelas tailored to both males and females who had not completed a screening. Patients received and digested vital communication about getting screened, where to find the nearest screening site, and more through culturally sensitive stories delivered in a familiar format.
A randomized control study found that 63% of patients who responded to the fotonovelas either liked or loved it, and 39% reported it positively impacted their willingness to act. By educating patients with curated content, AltaMed closed a key screening gap, lifted health literacy and perhaps most importantly – made significant progress toward health equity.
Notable Outcome
Patients that viewed the fotonovelas (19%) were more likely to submit a sample for cancer screening than patients in a control group (11%)
Best Use of Conversational A.I.
A Technology-Enabled Health Services Company
Program Goal
Promote smoking cessation among teen vapers
This leading health services organization employs over 210,000 employees globally and utilizes technology-enabled solutions to promote consumer wellness and population health. A major public health problem facing young adults, particularly teens, across the U.S. is the use of e-cigarettes, or vaping. The company sought to promote smoking cessation among teen vapers, a cohort still widely understudied, by implementing intelligent conversational solutions and educational content.
They collaborated with mPulse to build a personalized SMS program, lasting 4-6 months, that leveraged Natural Language Understanding (NLU) to deliver automated, interactive text dialogues to a targeted teen population. Individuals were also provided custom-built streaming health videos that offered tips on quitting and even an option to connect with an SMS coach.
The use of NLU enabled the delivery of automated messaging based on text responses, which helped the organization direct each individual to the appropriate resource. The program yielded an 85% engagement rate, and ultimately 69% of participating teens completed the program. The key result, that 73% of teens in the program set a date to quit vaping, demonstrates the value in utilizing automated text conversations and on-demand content to promote smoking cessation in vulnerable teens.
Notable Outcome
73% of participating teens set a quit date
Check out a new streaming health course for smoking cessation. »
Most Improved Consumer Experience
Program Goal
Increase Awareness of SNAP benefits (CalFresh)
CalOptima Health is a County Organized Health System that provides health insurance coverage for low-income children, adults, seniors and people with disabilities. As Orange County’s largest health plan, the organization includes a network of over 10,000 primary care doctors and serves over 900,000 Medi-Cal beneficiaries. The health system looked to address a gap they had identified with low-income families enrolling in the state’s food assistance program, CalFresh, federally known as SNAP.
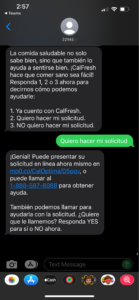
CalOptima and mPulse partnered to launch a two-way texting campaign, which utilized interactive SMS powered by NLU and tailored to 7 different languages. The health plan addressed language barriers by delivering vital information about CalFresh’s food security benefits to underserved families and Medi-Cal members in their preferred language.
Through automated text workflows, members could respond in their native language with answers like: “I already have CalFresh” or “I want to apply.” The program has continued to expand, having delivered over 5 million messages in 2022 already. Communicating with members according to their preferences about important CalFresh benefits helped CalOptima both improve consumer experience and reduce food insecurity for an at-risk population.
Notable Outcome
Over 5 million messages delivered to members in 2022 about CalFresh benefits
Like what you’re reading? Join us next year for Activate2023! Secure your spot now. »
Most Innovative Solution
Program Goal
Drive members to schedule a diabetic eye exam
Humana is one of the five largest health plans in the country according to member enrollment and has been partnered with mPulse for over 10 years. With more than 20 million members, including over 5 million Medicare members, the plan looked to close a gap with their members scheduling the annual diabetic eye exam.
The plan worked with mPulse to launch an SMS texting campaign to increase awareness around the importance of the eye exam and to drive members to schedule an exam. The program featured A/B testing, in which one half of members was provided a 30-second streaming health video in the initial message while the other half received only text.
The educational video enabled a learning experience that was easily accessible and familiar, concluding with a URL for members to learn more about scheduling the eye exam. Humana saw a remarkable 270% increase in clicks to schedule an exam when outreach included the streaming video. The test demonstrates that using streaming health content alongside two-way conversational solutions can significantly help activate hard-to-reach members with diabetes.
Notable Outcome
270% increase in clicks to schedule a diabetic eye exam when outreach included 30-second streaming video
Most Significant Outcome (tie)
A Technology-Enabled Pharmacy Services Company
Program Goal
Improve member experience and pharmacy engagement
The leading PBM and pharmacy services company is nationally recognized and fills over 1 billion prescriptions annually for millions of healthcare consumers across the country. With a rapidly growing population, the healthcare leader sought a solution to improve pharmacy patient engagement by utilizing a new communication channel for its home delivery pharmacy and prior authorization programs.
The pharmacy leader partnered with mPulse to roll out more than 50 outbound-dialer Interactive Voice Response (IVR) campaigns. The IVR messages notified members about prior authorization approvals/denials, refill reminders, shipping details and doctor responses.
Ultimately, over 5.8 million IVR records were exchanged and the outbound dialer launched over 5.1 million total calls. By offering a new avenue for members to complete a healthy action like ordering medications, the pharmacy enterprise initiated meaningful conversations to help enhance member experience, improve self-service capabilities, and close pharmacy engagement gaps.
Notable Outcome
Reached over 2.2 million members with 55,000+ members giving SMS consent
Most Significant Outcome (tie)
Program Goal
Improve refill adherence for HIV patients
MetroPlus Health Plan is a subsidiary of NYC Health & Hospitals, the largest municipal health system in the country. The insurance organization serves a diverse group of over 600,000 New York residents across Medicaid Managed Care, Medicare, D-SNP, MLTC and more plan types. A big challenge for the plan was getting HIV patients to refill medications that are pivotal to managing their condition and avoiding complications.

MetroPlus partnered with mPulse to educate the vulnerable population through interactive text messaging about the importance of medication adherence and reducing their unmedicated days. Texts were delivered one week apart and provided members with vital resources like phone numbers of a pharmacy or a member of the HIV care team.
The plan measured results based on whether or not a patient completed a refill within 7 days of initial outreach. The program yielded a 69% improvement in medication refills when SMS text reminders were deployed, indicating that text nudges inspire self-efficacy and action within this vulnerable population. Through targeted, mobile intervention, MetroPlus helped positively impact medication adherence for over 1,000 patients living with HIV.
Notable Outcome
69% improvement in medication refills with mPulse text reminders
Health Challenges in 2023
The 6 winners of this year’s Activate Awards showed that even when a new barrier is identified with engaging a population, healthcare organizations must adapt to adhere to their consumers’ needs. Whether utilizing a new communication channel, adding streaming video or incorporating multiple languages, the awards demonstrate that providing healthcare consumers with tailored, learning experiences can significantly impact how they engage with a program.
As the needs and preferences of healthcare consumers continue to evolve, so too should the capabilities of the healthcare organizations that serve them. Next year’s awards ceremony will surely exhibit a new string of engagement challenges with complex populations and niche use cases – let’s see what type of healthcare innovation surfaces in 2023!